Keloid Scarring
A keloid is an over aggressively healed wound. Basically, a keloid is an enlarged scar with a significant increase in collagen deposition. In normal skin, the collagen bundles basically run parallel and in a uniform manner. Keloids, on the other hand when evaluated by microscopy are noted to have no discrete collagen bundles. There is a diffuse, random organization of the collagen bundles with no significant regularity or associated relationship to the skin surface as seen with normal skin.
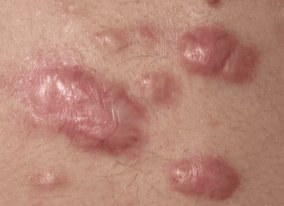
What is the cause of Keloid formation?
The incidence of keloid scar formation in human beings is much greater in darker skinned individuals and African-Americans. There is approximately a 15 times greater incidence of keloid formation in African-Americans than in Caucasians. One of the most significant aspects of keloid formation is that of its relationship to trauma or injury of the skin. Accidental or surgical injury to the skin is a predisposing factor to keloid formation. On the other hand, many keloids will form without any significant relationship to trauma, injury or surgery to the skin. The site of development of keloids is also of importance. There are specific areas of the body that are much more prone to keloid formation. The chest and presternal areas are significantly at risk for keloid formation. Also the shoulders and deltoid regions are commonly affected by keloids. Skin tension is a factor. Clearly, increased skin tension such as occurs in the shoulder area is a predisposing factor. On the other hand, the central portion of the face in and around the nose and lips is less likely and uncommonly is noted to have keloids.
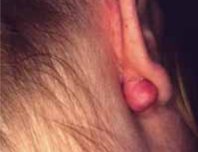
Treatment
Overall treatment for keloids of the skin is without significant success in all individuals. Multiple modalities have been tried and many have worked, but none have worked for all individuals.
Simple surgical excision and closure can cause a re-occurrence of the problem in approximately 80-90% of individuals.
Radiation therapy to the keloid healing site has also been met with some success, particularly when a certain amount of radiation (1,500 to 2,000 rads) are given to the healing site in the postoperative period.
Decreasing the skin tension can also benefit the keloids. Some physicians recommend skin grafting to the healing site so as to decrease the tension to the area and promote normal healing and lessen the chance for keloid formation.
Pharmacological management has been also utilized for keloid treatment. This has been met with some success. The benefits of pharmacological management is that surgery is not required. Radiation and other modalities can be invasive.
Intralesional injection with Triamcinolone tends to decrease the tendency for keloid and hypertrophic scar formation. A corticosteroid (eg, triamcinolone acetonide up to 40 mg/mL [up to 10 mg/lesion]) injected into the base of the lesion monthly (via a Luer-Lok syringe or by jet injection) may flatten the keloid but is often ineffective. Triamcinolone injection does carry some risk, including an increased tendency for depigmentation, telangiectasias, and associated dermal and skin atrophy
Other treatment modalities have included Retin 0.5% (Retin A which has been shown to somewhat decrease keloid size). Additionally, zinc oxide and antineoplastic agents such as Nitrogen mustard, Tetroquinone, and Thiotepa were utilized with some success.
C02 laser treatment to keloids has also been utilized and studied. There has been some improvement in reduction of the keloid formation with the C02 laser, however it is not noted in the majority of individuals.
Other treatments have included non-antibiotic moisturizing ointments.
Surgical treatments of choice
1. Intralesional excision and closure/skin grafting. The rationale behind this form of treatment is to leave the active peripheral portion of the keloid alone and excise the central dormant portions. With a smaller keloid primary closure is an option but for larger keloids a split thickness skin graft may be needed to close the defect. This particular form of treatment is thought to carry a 10-15% recurrence rate.
2. Surgical excision followed by radiotherapy. Surgical excision is followed in the immediate postoperative period by radiotherapy in either of three different forms. These are:-
- Sandwich radiotherapy – Radiotherapy is utilised before and after the surgical excision to dampen down activity of fibroblasts which are the cells responsible for collagen deposition and scar formation.
- Interstitial radiation – This involves the insertion of radioactive wires following excision. The wires are kept in place for a period of 48-72 hours when hospitalisation may be necessary.
- Surgical excision followed by fragmented surface radiotherapy. This appears to be the best current mode of treatment with an outpatient form of superficial radiotherapy over a period of four to five days.
However, it should be understood that there is no clear answer for keloid and hypertrophic scar formation. Some individuals simply have the tendency to develop keloids and despite surgical laser, chemotherapy, radiation therapy, or pharmaceutical agents, the keloids can persist.
Therefore, it is imperative that an individual understands the potential limitations of medical and surgical treatment for keloids and keep an open mind about overall potential success and more important the high risk of failure.